Key Takeaways
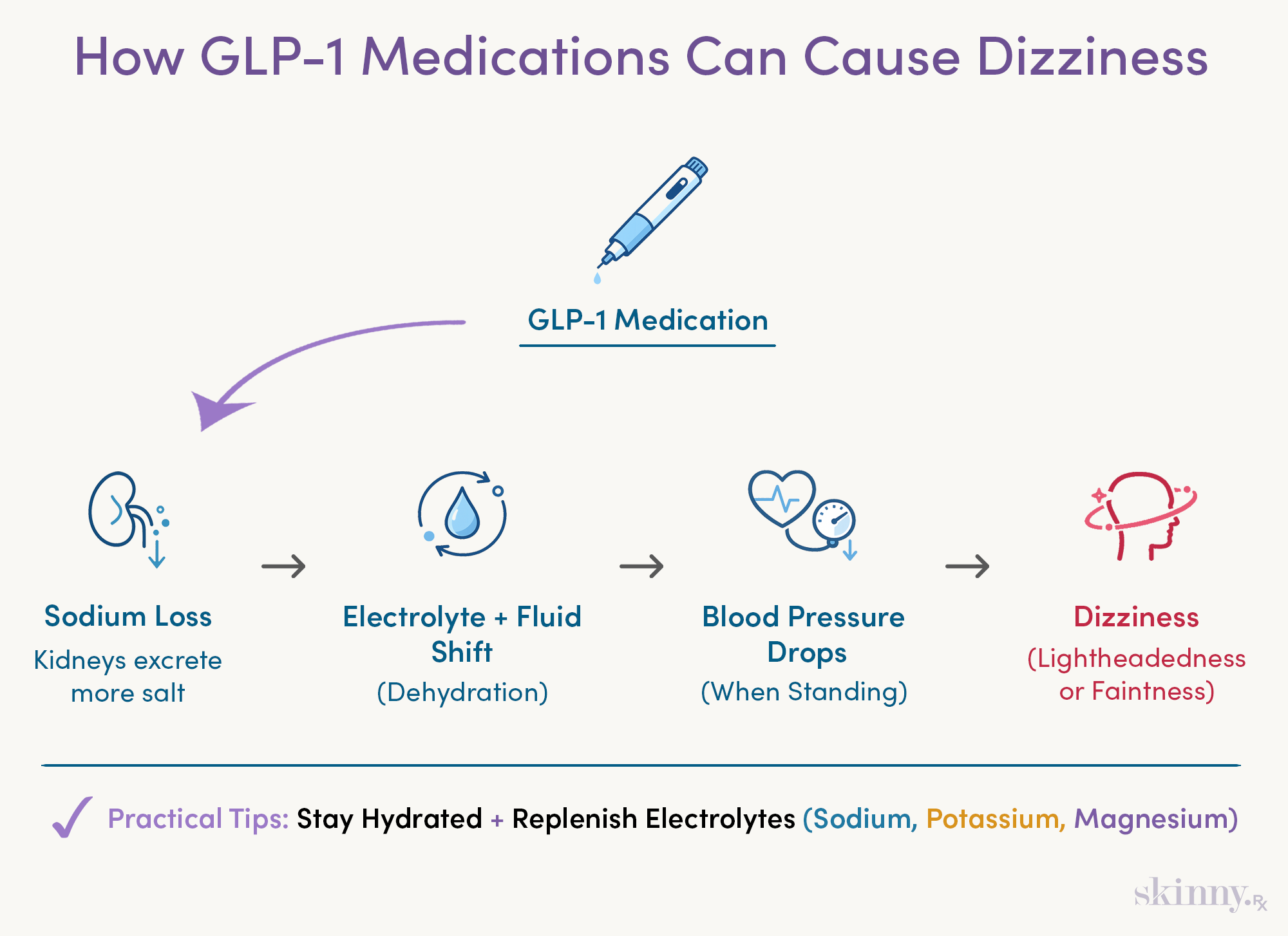
- GLP-1 medications can cause dizziness by altering fluid balance and increasing sodium loss through the kidneys, leading to temporary drops in blood pressure when standing.
- Drinking large amounts of water without replenishing electrolytes can worsen lightheadedness, since minerals like sodium help regulate circulation and hydration.
- Sodium, potassium, and magnesium support blood pressure stability, nerve signaling, and cardiovascular function when fluid balance shifts during GLP-1 treatment.
- Whole foods like fruits, vegetables, nuts, and seeds provide natural electrolytes, while supplements can help fill gaps when appetite changes or food intake declines.
- Timing hydration and electrolyte intake around GLP-1 injection days may help reduce dizziness, especially when nausea or reduced appetite disrupt normal eating patterns.
When it comes to GLP-1 side effects, gastrointestinal issues tend to steal the spotlight. But that doesn’t mean the dizziness you’re feeling on semaglutide or tirzepatide is all in your head. There’s a legitimate biological link between GLP-1 medications, fluid balance, electrolytes, and dizziness.
Dr. Daniel McGee, D.O., a board-certified family medicine physician and medical reviewer for SkinnyRx, says dizziness can occasionally appear in patients adjusting to GLP-1 therapy.
“Some patients taking GLP-1s can experience dizziness, especially if they’re not well-hydrated,” McGee explains. “I often remind my patients to pay attention to both food and electrolytes.”
Hydration matters—but so does the mineral balance that helps your body use that fluid properly.
Abrupt disorientation can be scary. Rest assured—spells of dizziness when taking medication aren’t always indicative of a more serious issue. Still, if you’re sick of being told to just “drink more water,” it may be worth looking beyond hydration alone. Electrolytes—the minerals that regulate fluid balance and blood pressure—can play an important role in why dizziness happens in the first place.
Why Do GLP-1s Cause Dizziness?
GLP-1s don’t make you dizzy on their own, but they can create certain downstream effects that ultimately contribute to feeling disoriented—especially when standing up quickly.
The mechanism at play here is called orthostatic hypotension: a sudden drop in blood pressure in your torso and head when you stand, due to your heart’s inability to pump blood upward fast enough to overcome gravity, causing lightheadedness and brain fog.
For most GLP-1 users, standing head rushes are the most common form of dizziness and dissipate after a few moments. However, that doesn’t mean they aren’t inconvenient or fine to ignore at all times.
The Kidney Connection
Gravity isn’t the sole culprit of lightheadedness on semaglutide or tirzepatide. GLP-1s have several effects on your kidneys, including a process called natriuresis, which signals the kidneys to excrete more sodium through the urine.
While natriuresis is a normal biological function of healthy kidneys, GLP-1 drugs appear to modestly enhance this process. This can increase sodium and water excretion and may slightly reduce circulating blood volume. In some people, especially if fluid intake is low or gastrointestinal side effects are present, this shift can contribute to feelings of dizziness or lightheadedness.
Too Little Food, Too Much Water
For most people, “drink more water” is sound health advice and a smart way to tackle dizziness or headaches. After all, most people eat a lot of high-sodium foods, and don’t drink enough water to properly hydrate.
If you’re experiencing head rushes on Ozempic or Wegovy, you may have the opposite problem. Here’s what might be happening:
- Proper hydration is about balancing your fluid and mineral intake, not just chugging plain water.
- GLP-1s facilitate weight loss by regulating appetite; people tend to eat less often, and consume smaller portions, while keeping water intake high.
- Electrolytes like sodium help maintain proper blood pressure and circulation. But with too much raw material (water) and no workers (electrolytes), your heart can’t react appropriately to external pressure forces like gravity.
The end result is feeling like you’re about to fall over every time you stand up while taking a GLP-1, despite sticking to the commonly repeated—and sensible—advice of drinking plenty of water.
The good news? You can tackle orthostatic hypotension and avoid over-hydration with a quick trip to the supplement cabinet.

Clarity for Your Health Goals
Answer a few questions to connect with licensed providers who, if appropriate, can prescribe weight loss medications to support your health goals.
Electrolytes for GLP-1 Dizziness: The “Big 3” Essential Minerals
When you take a GLP-1, your body works more like a sieve or a filter rather than a sponge. The medication encourages your body to dump sodium reserves, leaving less ionic material to regulate your water levels.
Sodium is one of three major electrolytes that act like organic netting, “catching” the water you drink and ensuring it properly hydrates and restores blood pressure. They aren’t a cure-all, but if you’re deficient in these essential minerals, prioritizing electrolytes can help manage things.
Why are they considered “essential”? Because you need to get them from food sources as your body cannot produce electrolytes naturally.
Sodium
Sodium catches a bad rap in the wellness industry. Excessively salted foods certainly aren’t good for you in abundance, but sodium is an essential mineral—and it’s found in table salt.
Too much salt is a risk factor for those with chronic hypertension, which some GLP-1 medications are used to treat. However, rapid weight loss risks sodium deficiency. In such cases, you may need to intentionally reintroduce sodium to balance things out.
Potassium
Just as water intake and electrolytes balance each other out, potassium, another essential mineral, helps balance out the harmful effects of sodium. And if you’re deficient in potassium, you’re at risk of hypokalemia, which may cause you to feel dizzy or faint.
Magnesium
Magnesium supports healthy cardiovascular function, cellular repair, muscle contractions, and also works synergistically with other electrolytes. While true magnesium deficiency is rare, some clinical data do show that insufficient levels encourage neurological symptoms like fainting, especially in older patients.

Some patients taking GLP-1 medications can experience dizziness, especially if they’re not staying well hydrated. I often remind my patients to pay attention to both fluids and electrolytes, but also to be mindful of sodium intake. Some electrolyte drinks contain close to 1,000 mg of sodium per serving, so it’s easy to overshoot the generally recommended upper limit of about 2,300 mg per day.
–
Dr. Daniel McGee, Board-certified Family Medicine Physician
Best Electrolyte Sources for Semaglutide and Tirzepatide
You can get more electrolytes in one of two ways: adjusting your dietary habits or incorporating a supplement. Which one is right for you will depend on your lifestyle, financial means, and even your GLP-1 dosage.
Supplements vs. Whole Foods
Here’s the short answer: Whole foods are a better source of vitamins and minerals than dietary supplements, if all other factors are kept equal. Natural, unprocessed foods contain all the essential micronutrients you need, plus phytonutrients, fiber, and more.
On paper, you shouldn’t need an electrolyte supplement—if you have the perfect diet. The crux of the issue is that most people do not have the means, financially or logistically, to always eat a diverse, nutrient-dense, whole-foods based diet.
Not to mention the fact that some people experience palate narrowing while on GLP-1s, making it harder to diversify their plates, explains Dr. McGee.
Supplements are meant to fill those dietary gaps, not substitute whole foods altogether. Foods high in electrolyte content include leafy vegetables, fruits, and certain nuts and seeds. If those sources are inaccessible, an electrolyte supplement can help, but it isn’t mandatory.
What To Look for in a Powder (and What To Avoid)
When considering any supplement purchase, you need to start with the big three:
- Price: Is it within reach financially, and is it a more cost-effective option than the next best alternative?
- Formulation: Does it contain the desired ingredients in sufficient quantities, and have they been sourced appropriately?
- Presentation: Do you enjoy the taste, texture, and sensory experience enough to consume it regularly?
Price and presentation are personal decisions. When it comes to formulation, look for powders or drinks that have sodium (100-500mg), potassium (1,600-3,500mg), and magnesium (300-420mg).
Managing GLP-1 Dizziness Around Injection Days
Opening your wallet for an electrolyte supplement isn’t the only thing you can do to get more electrolytes for GLP-1 dizziness, especially if you feel lightheaded on or around your injection day.
Clinical data does not indicate that injecting semaglutide induces acute dizziness. That said, side effects (including brain fog, lightheadedness, or fainting) often present a day or two after injection, especially if you’re still titrating your dosage.
Not to mention the act of injecting itself can be nerve-wracking. Electrolytes are not guaranteed to prevent dizziness or fainting, but consuming them on injection day, several hours before your shot, might help.
You should also continue to hydrate and replenish both water and essential minerals in the two days after your injection, particularly if you’re prone to nausea or other issues that hamper normal eating habits.
Frequently Asked Questions

Considering GLP-1s for Weight Loss?
If you’re exploring medications like semaglutide or tirzepatide, start with a quick assessment at SkinnyRx. A licensed clinician will review your health profile, help determine the safest and most effective path forward, and provide ongoing support throughout your journey.


 Medically Reviewed
Medically Reviewed



