Key Takeaways
- Popular GLP-1 medications can cause food aversions, where certain foods suddenly feel unpleasant or difficult to tolerate due to changes in taste, smell, or texture.
- Food aversions are often most noticeable during the early stages of treatment and may improve, stabilize, or change over time as your body adjusts to the medication.
- Eating smaller, more frequent meals and choosing foods that feel easier to tolerate can help maintain proper nutrition while managing food aversions.
- Cold or minimally heated foods often trigger fewer food aversions because they release fewer aromas, making them easier to eat comfortably.
- Persistent food aversions that prevent you from eating enough can lead to fatigue, weakness, or other signs of undernutrition and may require guidance from a healthcare provider.
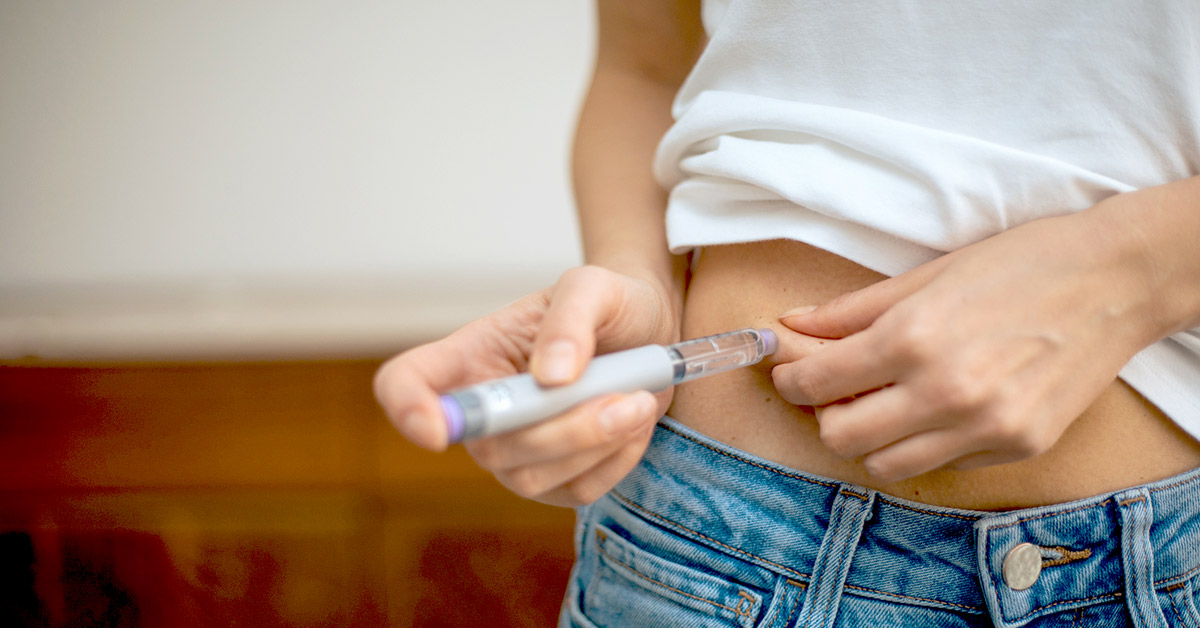
Many people taking GLP-1 medications notice changes in appetite, taste, and food preferences. In some cases, this can include developing strong negative reactions to certain foods. Foods that you used to crave may seem less appealing, and on the more extreme end, may even trigger gastrointestinal symptoms like nausea or vomiting.
Some GLP-1 users report strong food aversions, or strong aversions to specific foods, often driven by the smell or taste. A food aversion is a learned or conditioned avoidance of a specific food, where the brain begins to associate that food with an unpleasant or undesirable experience.
Taste and smell play an important role in sensing nutrients, regulating metabolism, and influencing how much and what we choose to eat. Most of us are familiar with the five senses: taste, smell, touch, sound, and sight. Taste isn’t just about detecting specific flavors on your tongue; it’s a complex body process that helps connect what we eat with how our bodies respond.
Flavor is created by the combination of three senses: taste, smell, and the body's somatosensory system that interprets our senses. The system of taste buds and nerves recognizes five basic tastes — sweet, sour, salty, bitter, and umami. Umami is usually described as a meaty, earthy, or savory flavor.
This guide explains why GLP-1 medications can cause food aversions and provides practical strategies to help you maintain proper nutrition and eat more comfortably while on treatment.
The "I Can't Even Look at It" Phase: Understanding GLP-1 Aversions
Taste changes are common with GLP-1s, but the degree of change is a spectrum. Some people may simply experience decreased cravings, while others may experience strong food aversions, especially in the early phases of taking the medication.
In one study, participants on liraglutide reported decreased cravings for sweet, salty, savory, or fatty foods. In another study, women on semaglutide were able to recognize more flavors than those on a placebo and had altered brain responses to sweet and savory foods.
The Brain-Gut Rewiring: Why Your Cravings are Muted
You may be familiar with the gut-brain connection, or the signaling that occurs in both directions between the brain and the gastrointestinal tract. With the rise in the use of GLP-1s, researchers are now exploring a gut-brain-taste connection to describe the crosstalk between individual perceptions of tastes, cravings, aversions, hunger and satiety hormones, levels of nutrients in the blood, and nutrient stores in the body.
Many GLP-1 users report reduced “food noise,” making their weight-loss journey feel more manageable. Food noise describes the constant and intrusive thoughts about food.
Though the exact mechanism is unknown, GLP-1s seem to soften or mute food noise, similar to turning down the dial of a stereo.
Taste Aversions: Why Your Sense of Taste May Be Changing
Some GLP-1 users report dramatic changes in their taste preferences. A favorite food, such as a juicy cheeseburger, may suddenly be a turn-off. This may be caused by several factors, such as increased nausea from high-fat foods.
Additionally, GLP-1s may directly impact food cravings or aversions by impacting the expression of taste receptors on the tongue.
In one study, participants on semaglutide had reduced cravings for salty, spicy, starchy, and dairy foods compared to a placebo. GLP-1s may even improve your ability to recognize a range of flavors, which can then make you more sensitive to food aversions.
Ultimately, taste is individualized because it depends on a mix of complex factors, so your food aversions may change in unique ways.
Common Aversions: Why Coffee, Meat, and Alcohol Top the List
Receptors for the natural hormone, GLP-1, are expressed in the taste buds on your tongue. When taken as a medication, GLP-1s can impact your sense of taste in specific ways. Though the experience of taste is somewhat individualized and subjective, many people report aversions to certain foods such as coffee, meat, or alcohol.
The Metallic Taste: Dysgeusia and GLP-1s
Many different medications may cause dysgeusia, a condition of experiencing a foul, salty, rancid, or metallic taste. Taste changes may also be impacted by other medical conditions; for this reason, it is important to share your symptoms with your physician.
Helpful Hacks: Reducing Off Tastes
If experiencing a change in tastes, you can experiment with different strategies:
- Hydrate, hydrate, hydrate: Drinking plenty of water throughout the day will prevent dry mouth, which can worsen dysgeusia.
- Focus on oral hygiene: Regular brushing and flossing of your teeth may help prevent or manage dysgeusia by reducing oral bacteria.
- Mouth rinse: Try rinsing with a solution of baking soda and water to neutralize acids in your mouth.
- Utensil swap: Exchange metal utensils and water bottles for glass or plastic versions.

Support for Your Weight Loss Journey Starts Here
SkinnyRx helps you start GLP-1 treatment with licensed doctors who guide and support you along the way, including managing side effects like food aversions. Take the online assessment to see if you’re eligible and begin with care designed to help you succeed.
Tactical Strategies for Maintaining Nutrition
While managing any new food aversions, several strategies can help to minimize triggers and ensure you are meeting your nutrient needs.
The "Safe Food" List: Building Your Menu for Success
You can manage food aversions while still following a healthy dietary pattern. Build your meals around nutrient-dense foods that are well-tolerated. A healthy dietary pattern includes:
- Vegetables: Choose a variety of differently colored vegetables (e.g. dark green, red/orange, red, orange, and purple), while limiting those that tend to have strong smells during cooking (e.g. Brussels sprouts, cauliflower, cabbage)
- Fruits: Enjoy fruits of all colors, such as red, green, blue, purple, or yellow. Add frozen fruits to smoothies or shakes if well-tolerated.
- Whole grains: Grains tend to have relatively mild flavors, and may therefore become a favored food group. Focus on whole grains (e.g., oatmeal, barley, whole wheat, quinoa, brown rice, whole grain cornmeal) and minimize refined grains (e.g., white flour, crackers, bread products made with refined flour).
- Lean protein: Adequate protein is critical while on GLP-1s. Protein sources can be plant-based (e.g., beans, legumes, nuts, seeds) and animal-based (e.g., fish, poultry, beef, lamb, pork, dairy, eggs). To reduce flavors from animal-based proteins, try eating them cold instead of warm (e.g. chicken that has been cooked and cooled).
- Healthy fats: Choose healthy fats when cooking (e.g., olive oil, sunflower oil). Nuts and seeds are also good sources of both healthy fats and protein.
Avoiding the "Cooking Cloud": Managing Kitchen Smells
Foods release aromas when they are cut (e.g. sliced onion) or heated (e.g. bread baking in the oven). Sometimes, simply being in the kitchen near strong food aromas can be a turn-off.
To minimize this effect, you can cook foods in the oven rather than on the stovetop, use the hood on your stove to remove strong odors, prepare foods outdoors if the weather is agreeable, or open the windows in your kitchen.
Temperature Hacks: Why Cold Foods Often Bypass Aversion
One easy hack to reduce food aversions is to eat cold foods. Your sense of taste is strongly influenced by your sense of smell. Food releases scent particles that travel into the nasal cavity and send signals to the brain.
More particles are released when food is heated, making its smell stronger. Eating mostly cold foods can help to minimize their aromas, and therefore reduce an aversion.

Routine Eating: Shifting Your Relationship with the Plate
Though you may have relied on your body’s natural hunger and satiety cues before starting GLP-1s, the medication is known for its appetite-suppressing effects. Coupled with taste changes, this may put you at risk for poor nutrition.
Scheduling vs. Intuition: When to Stop Waiting for Hunger
Following a stable, consistent dietary pattern is an important way to ensure you are meeting your nutrient needs. Choose small, frequent meals every 2-3 hours to help with nausea and other gastrointestinal upset. These meals should be built around lean protein sources, vegetables, fruits, whole grains, and healthy fats.
A sample dietary pattern with small, frequent meals may include:
Energy-Dense Liquid Nutrition as a Bridge
If you are unable to tolerate solid foods at first, energy-dense liquid nutrition may be a helpful bridge until your symptoms resolve. Liquid meals can be an effective way to pack in nutrients and calories in a small volume.
Aim for small liquid meals at a time, such as 6-8 fl oz every hour, in order to prevent gastrointestinal upset. These may include shakes or smoothies with yogurt, fruit, and vegetables. Oatmeal and nut butters can also be pureed into shakes to incorporate whole grains and healthy fats.
If the odor of certain liquids is nauseating, consider drinking through a straw placed in a container with a lid. The odors from the liquid will be muted when compared to drinking from an open cup.
When to Be Concerned: Malnutrition vs. Healthy Satiety
Though temporary swings in appetite or food aversions aren’t likely to be harmful, long-term changes that significantly reduce your appetite may compromise your health.
If you aren’t able to eat enough food to meet your nutrient needs, your body may start to let you know it’s not getting enough energy with specific signs and symptoms. Some signs may show up within a few weeks (e.g., fatigue, weakness, brain fog, dizziness, headaches, constipation) while others may take months to manifest (e.g., changes in the health of your hair, skin, and nails, poor wound healing, or frequent infections).
If you suspect you aren’t eating enough to meet your needs, consult with your physician and a registered dietitian as soon as possible. Your healthcare providers may help by adjusting your medications, strategizing to manage your symptoms, or determining solutions to meet your energy and nutrient needs.
Support Every Step of Your GLP-1 Weight Loss Journey
Food aversions are a common side effect of GLP-1 medications like semaglutide or tirzepatide, and managing them properly can help you stay consistent and continue making progress.
At SkinnyRx, licensed doctors prescribe GLP-1 treatment and support patients throughout their weight loss journey, helping you manage side effects and stay on track. You can take the online assessment to get started and see if treatment is right for you.


 Medically Reviewed
Medically Reviewed