Key Takeaways
- Semaglutide and other GLP-1 medications are now used beyond weight loss to improve outcomes in certain heart failure patients, especially HFpEF.
- Benefits extend beyond weight loss, including reduced inflammation, improved metabolic function, and better overall heart performance.
- Clinical studies show improvements in symptoms such as shortness of breath and physical limitations, as well as quality of life.
- Results are gradual, with improvements typically appearing over weeks to months.
- Treatment should be guided by a healthcare provider to ensure safety and proper coordination of care.
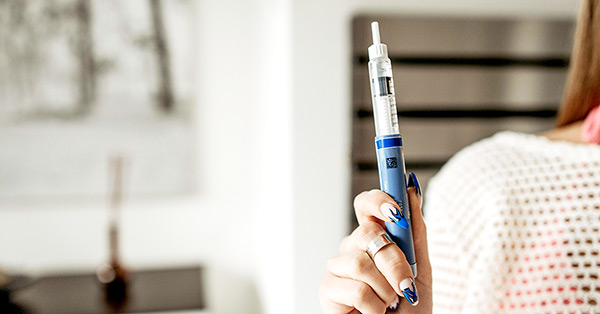
GLP-1s are most commonly known as medications for weight loss and blood sugar regulation. Yet a few (Wegovy, Victoza, and Trulicity) are also FDA-approved for preventing life-threatening cardiovascular events, such as heart failure.
But what exactly is the connection between this medication class and heart health? Ahead, we’ll answer that question, reveal recent research on heart failure and GLP-1s, and outline when it’s time to talk to a cardiologist about this medication type.
A New Era for Cardiology: Why Semaglutide is a "Heart Drug"
GLP-1 receptor agonists are a medication class that mimics the naturally occurring GLP-1 hormone. This hormone plays a role in blood sugar regulation and weight management, though GLP-1 medications may provide other benefits too, including for heart health.
For over a decade, researchers have run cardiovascular outcomes trials with GLP-1s. Initially, they conducted these trials to determine if GLP-1s were safe for people with heart conditions, but the results suggested these medications may reduce the risk of deaths due to heart disease, non-fatal strokes, and some types of heart failure.
These findings led the FDA to approve Ozempic for cardiovascular use as a “heart medication” in 2020, followed by Wegovy in 2024. More specifically, Ozempic’s FDA label says it may reduce the risk of adverse cardiovascular events in those with established cardiovascular disease risk factors and/or type 2 diabetes. Wegovy’s updated FDA labels say it may reduce the risk of adverse cardiovascular events in those with established cardiovascular disease risk factors and/or obesity.
Soon after Wegovy’s updated approval, the FDA approved Trulicity and Victoza for the same purpose.
"We used to think of GLP-1 medications primarily as diabetes drugs and later as weight-loss drugs,” says Sajad Zalzala, MD, a board-certified family medicine physician, “What we’re now discovering is that they’re really metabolic medicines. When you reduce inflammation, visceral fat, and insulin resistance all at once, the heart often benefits in ways we didn’t fully anticipate."

We used to think of GLP-1 medications primarily as diabetes drugs and later as weight-loss drugs. What we’re now discovering is that they’re really metabolic medicines. When you reduce inflammation, visceral fat, and insulin resistance all at once, the heart often benefits in ways we didn’t fully anticipate.
–
Dr. Sajad Zalzala, MD, SkinnyRx Medical Director
The Science of the "Stiff Heart"
Heart failure is one of the most common cardiovascular diseases, impacting almost 6.7 million Americans. This condition refers to when someone’s heart doesn’t pump the oxygen and blood required by other organs.
There are two types of heart failure:
- Heart failure with reduced ejection fraction (HFrEF): When the heart isn’t pumping enough blood into circulation, it’s referred to as HFrEF or systolic failure.
- Heart failure with preserved ejection fraction (HFpEF): Sometimes called diastolic heart failure, this is when the necessary blood doesn’t fill the heart between each beat, though blood is still being pumped into circulation.
Over 50% of patients are diagnosed with HFpEF, which is usually less severe than HFrEF. However, if HFpEF is left untreated, it can progress into HFrEF. Heart failure with preserved ejection fraction is sometimes referred to as a “stiff heart,” and it greatly reduces someone’s quality of life. It can lead to feeling tired faster when working out or being physically active, trouble concentrating or thinking, and chest pain.
How GLP-1s Help with HFpEF
When someone is diagnosed with HFpEF, treatment often focuses on improving overall quality of life and stopping the progression to HFrEF. Until recently, HFpEF had limited treatment options. Now, GLP-1s could change that. In clinical trials, GLP-1s reduced symptoms of HFpEF, and a 2026 meta-analysis of these trials points out that GLP-1s may improve quality of life.
Plus, these medications’ effects may be even more pronounced for people with certain heart failure risk factors. These include obesity, type 2 diabetes, high inflammation levels, and too much epicardial adipose tissue.
Effect on Obesity and Type 2 Diabetes
GLP-1s are most commonly prescribed for blood sugar regulation and obesity. Blood sugar is absorbed by cells to be used as energy. After someone eats, GLP-1 (whether naturally occurring or via a medication) triggers the release of insulin, which helps those cells absorb blood sugar.
However, in those with prediabetes or type 2, the body’s cells are less responsive to insulin, and blood sugars rise. GLP-1 medications bind to GLP-1 receptors and trigger the body to produce more insulin, which can help blood sugar be absorbed by those cells.
When the medication bonds with GLP-1 receptors, it slows gastric emptying, making someone feel full for longer. GLP-1 may also decrease hunger hormones and appetite. In turn, this has led to meaningful weight loss for many people.
Reducing Epicardial Adipose Tissue
Another important risk factor for HFpEF is epicardial adipose tissue, which is fat tissue located around the cardiovascular system. High levels of this tissue increase the risk for heart failure in the first place, though it may also make symptoms worse and speed up heart failure progression in those who already have HFpEF.
Epicardial adipose tissue has GLP-1 receptors, making it a prime candidate for GLP-1 medication’s effects. In studies and meta-analyses, it’s well-documented that GLP-1s reduce this fat tissue.
Systemic Inflammation: The Silent Driver of Heart Failure
The relationship between inflammation levels and heart failure is complicated. Researchers are still trying to figure out how this relationship works, though there does seem to be a correlation between high inflammation levels and heart failure.
GLP-1s may reduce systemic inflammation. One way to measure inflammatory levels in the body is to look at C-reactive protein (CRP) levels. In some clinical trials, the CRP levels decreased by an average of 43% after participants took a GLP-1 medication.
What the 2026 Clinical Updates Tell Us
One of the biggest clinical trials on semaglutide and heart failure was the STEP-HFpEF trial. This study included 58,333 patients and compared semaglutide to a placebo. Those on semaglutide experienced a 40% reduction in hospitalizations and all-cause mortality. Many also reported an improved quality of life and fewer heart failure symptoms.
The STEP-HFpEF Trials: Weight Loss vs. Direct Cardiac Benefit
The STEP-HFpEF trial demonstrated three main semaglutide benefits:
- Fewer symptoms of HFpEF
- Fewer physical limitations in day-to-day life
- A reduction in body weight
A main drawback of this trial is it didn’t explain the mechanisms behind these improvements, and there are some questions as to whether GLP-1s lead to direct cardiac benefits or if these benefits are due to weight loss and reduced inflammation, which can both make heart failure worse for those who are already diagnosed with heart failure and are risk factors for developing this condition in the first place.
Why Ejection Fraction Matters (And Why It Stays "Normal" in HFpEF)
A smaller clinical trial suggests GLP-1 medications do not have the same impact on HFrEF. This may be due to the fact that GLP-1s may increase heart rate, though researchers are still looking into what the American Heart Association refers to as an “uncertain safety profile” for people with HFrEF.
Real-World Results: More Than Just a Number on the Scale
GLP-1s may mitigate the risk factors of heart failure and reduce symptoms or slow the progression of HFpEF, with clinical research showing marked improvements for participants with heart failure who take a GLP-1.
That improvement is felt beyond the number on the scale:
- Improvement on the 6-minute walk test: This test assesses how far someone can walk in six minutes, which is a measure of aerobic health. People with HFpEF who took a GLP-1 medication could walk further, with a mean change of 21.5 meters more in six minutes after taking semaglutide.
- Fewer symptoms: The Kansas City Cardiomyopathy Questionnaire (KCCQ-CSS) measures a patient's cardiovascular symptoms, with a higher score meaning someone is experiencing fewer symptoms and physical limitations. In multiple studies, the scores of patients on GLP-1s improved, meaning GLP-1s may reduce heart failure symptoms and effects on everyday life.
- Improved functional capacity: HFpEF’s symptoms negatively impact someone’s functional capacity. In some studies, a GLP-1s medication improved functional capacity, meaning heart failure wasn’t holding patients with heart failure back as much in their day-to-day life.
Safety and Coordination: Working with a Cardiologist
GLP-1s are a prescription medication, meaning someone can’t walk into a drug store and buy them without a written prescription from a healthcare provider. For those with HFpEF or those who are at a higher risk for this condition, the prescribing doctor is often a cardiologist.
Monitoring Heart Rate: What You Need to Know
GLP-1s increase heart rate, and a cardiologist may ask you to track your heart rate when on a GLP-1. For those with HFpEF, the benefits of these medications may outweigh the heart rate increase, so long as it’s closely monitored. However, this might not be the case for everyone or for those with HFrEF, which is why it’s important to work with a cardiologist.
Combining GLP-1s with Beta-Blockers
Before taking any medication, a healthcare provider looks at how it may interact with other drugs you’re already taking. However, not all drug interactions are bad.
A beta-blocker, for example, is commonly prescribed for HFpEF and is safe to take alongside a GLP-1. It may even lower the heart rate of patients who take a GLP-1 medication, limiting a potential cardiovascular concern of GLP-1s.


 Medically Reviewed
Medically Reviewed